Article Text
Abstract
Background Aetiology of births involving very low birthweight (VLBW) and extremely low birthweight (ELBW) infants is heterogeneous and preventive strategies remain elusive. Socioenvironmental measures implemented as Ireland’s response to the SARS-CoV-2 virus (COVID-19) pandemic represented a national lockdown, and have possibly influenced the health and well-being of pregnant women and unborn infants.
Methods Regional trends of VLBW and ELBW infants in one designated health area of Ireland over two decades were analysed. Poisson regression and rate ratio analyses with 95% CI were conducted. Regional data covering most of the lockdown period of 2020 were compared with historical regional and national data and forecasted national figures for 2020.
Results Poisson regression analysis found that the regional historical VLBW rate per 1000 live births for January to April, 2001–2019 was 8.18 (95% CI 7.21 to 9.29). During January to April 2020, an unusually low VLBW rate of just 2.17 per 1000 live births was observed, reflecting a rate ratio of 3.77 (95% CI 1.21 to 11.75), p=0.022, representing a 73% reduction of VLBW during the first 4 months of 2020 compared with same period for the preceding two decades. There were no ELBW infants admitted to the regional neonatal intensive care unit. National Irish VLBW rate for 2020 is forecasted to be reduced to approximate 400 per 60 000 births compared with the historical 500–600 range.
Conclusion An unprecedented reduction in regional births of VLBW and ELBW infants was observed in Ireland coinciding with the COVID-19 lockdown. Potential determinants of this unique temporal trend possibly reside in the summative socioenvironmental impact of the COVID-19 lockdown. Our findings, if mirrored in other regions that have adopted a lockdown, demonstrate the potential to evaluate these implicated behavioural and socioenvironmental modifiers to positively influence VLBW and ELBW rates globally.
- child health
- maternal health
- obstetrics
- paediatrics
- public Health
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/.
Statistics from Altmetric.com
Key questions
What is already known?
Very low birthweight (VLBW) and extremely low birthweight (ELBW) infants contribute significantly to under 5 mortality globally.
Currently, there is no broadly accepted and effective strategy to prevent the birth of premature VLBW and ELBW infants.
Impact of cumulative socioenvironmental and maternal behavioural modifications on the incidence of very preterm births has not been assessed.
What are the new findings?
COVID-19-triggered national lockdown in Ireland created an opportunity to study the cumulative influence of socioenvironmental modifications on pregnant mothers.
An unprecedented 73% reduction in live births of VLBW infants and a 100% reduction of ELBW infants were noted in one designated health region of Ireland during January to April 2020 compared with the preceding 20 years.
Our observations, if nationally mirrored, indicate that birth rate of VLBW and ELBW infants in Ireland is forecasted to decrease considerably in 2020.
Key questions
What do the new findings imply?
Our observations, if reflected in other countries that adopted COVID-19- prompted lockdown measures, could redefine the antecedents that trigger the yet poorly understood pathways leading to very low birthweight (VLBW) and extremely low birthweight (ELBW) births.
Socioenvironmental alterations, maternal behavioural modifications, ease of access to maternity services and the enforcement of lockdown measures could impact variably during pregnancy in different regions of the world.
Reducing VLBW and ELBW rates would be the most important ‘curve to bend’ to reduce infant mortality globally and thus promote the achievement of sustainable development goals for children.
Introduction
Over 15 million babies are born too early, too sick and too small in the world annually. One million of these infants die.1 Very low birth weight (VLBW <1500 g) and extremely low birth weight (ELBW <1000 g) contribute significantly to infant mortality.2–5 In 2016, 46% of the under 5 mortality globally was contributed by neonatal deaths within the first 28 days of life and the main contributor was prematurity.5 VLBW and ELBW rates are increasing in most of the developed, middle-income and low-income countries and a significant proportion are of unknown aetiology.2 6 The frequency of preterm birth (PTB) varies from 5% to 9% in Europe, 10.6% in North America to 11.9% in Africa.7 8 Most VLBW and ELBW infants are born to women with no prior history of premature births.5 9
Prevention of VLBW and ELBW births is considered a public health priority. Despite growing relevance, progress has been modest.10 Currently, there is no standardised and effective strategy to prevent VLBW and ELBW births, and implementation of socioenvironmental approaches to mitigate the risk of such deliveries would require better elucidation of non-medical factors that are both under-recognised and underevaluated.11 Although the causal biological mechanisms mediating such births are poorly understood, preterm premature rupture of membranes (PPROM), amniotic inflammasome mediation, alterations to vaginal microbiota, variations in cytokines, chemokines and other inflammatory modulators, as well as intra-amniotic inflammation and infections have been suggested as the biological antecedents.12–15 Recognising the sources of heterogeneity and phenotypic plasticity in VLBW and ELBW births may inform eventual effectiveness of preventive measures.16 17
Socioenvironmental measures implemented as Ireland’s response to the SARS-CoV-2 virus (COVID-19) pandemic collectively constituted a national lockdown, and may possibly have influenced the health and well-being of pregnant women and their unborn infants. In that specific setting there existed an opportunity to compare the trend of VLBW and ELBW rates during the lockdown period with the historical data. Potential influence of a multitude of biological, physical and environmental factors could cumulatively modify the births of VLBW and ELBW infants. We wished to assess whether these redefined social and behavioural boundaries have fostered an environment favourable to influence the VLBW and ELBW birth rates. These few months offered a unique opportunity to study the effects of a ‘Nature’s experiment’ of non-medical, behavioural and socioenvironmental alterations as potential determinants influencing overall health of the ‘intrauterine habitat’.
Methods
Setting
A nationwide lockdown was implemented in Ireland on 12 March 2020 in response to the COVID-19 pandemic and continued till 18 May. This reflected the shutdown of offices, shops, colleges, schools, childcare facilities and all other institutions deemed non-essential. Traffic and mobility restrictions were imposed and most of the workforce adapted to a new work-from-home (WFH) model. The Irish government advised the population from mid-February 2020 to follow strict hand hygiene measures, social distancing and adherence to WHO recommendations to reduce COVID-19 transmission.
Irish COVID-19 lockdown was lifted in a phased approach from 18 May; although most non-essential services remained closed with ongoing mobility and social restrictions till 29 June (end of phase 2). However, we have maintained our observations till the end of June 2020 (half of the year). This period of phased easing of the socioenvironmental measures facilitated ascertaining whether the observed VLBW and ELBW trends sustained or reverted immediately at the end of full lockdown in 2020.
Study population
University Maternity Hospital Limerick (UMHL) is the only maternity facility for a population of 473 000 from the counties of Limerick, Clare, North Tipperary and nearby catchment areas. It provides an opportunity to analyse the demographic and epidemiological trends of births involving VLBW and ELBW infants of one of the designated health regions in the Ireland.18 All VLBW and ELBW infants of the region from 22 weeks of gestation are treated locally (apart from surgical or cardiac interventions). Perinatal demography and patient characteristics of the study population have been published previously.19 All VLBW and ELBW live births at UMHL from 1 January 2001 to 30 April 2020 were included in the study. No cases were excluded based on congenital anomalies, multiple gestations or inconsistencies around the accuracy of gestational age (GA) estimation.
There were no overarching significant alterations to the antenatal, obstetric or intrapartum care pathways initiated for the pregnant women at UMHL from January to April 2020 compared with preceding 5 years. Policies on antenatal steroids, antenatal magnesium sulphate, resuscitation of ELBW infants at the margins of viability, frequency of antenatal visits and obstetric ultrasound scans, peripartum maternal antibiotics for group B streptococcus prophylaxis, maternal sepsis management (sepsis six) and the Irish maternity early warning system were operational. Of note, over a 20-year span, internationally accepted and evidence-based practices were implemented at UMHL compliant with national-level and local-level obstetric and neonatal guidelines.
Birthweight-based data capture and analysis
There are two established methods for cohorting high-risk infants, by birth weight or GA.20 A birthweight-based analysis was chosen for this study, and not primarily based on very low GA (VLGA, <32 weeks). VLBW could be through pure prematurity, a combination of prematurity and growth restriction/small for GA (SGA) or much less commonly through intrauterine growth restriction (IUGR) alone. We have chosen to study the VLBW and ELBW trends considering the following factors, (1) Accurate institutional data and monthly statistics spanning over two decades was collected primarily on weight-based criteria and later only GA added, (2) GA was calculated based on the best obstetric estimate and varied over decades based on last menstrual period, early prenatal ultrasound (dating scan or booking scan) or a combination, (3) For the first few years of historical data GA was adjusted to completed weeks (26 or 28 weeks) and not to exact days (25+5/7 or 28+2/7), (4) To facilitate later international comparison including low/middle-income countries having more SGA contribution and that the dating scan-based accurate GA assessment may not be always available, and (5) To facilitate future international benchmarking studies through Vermont Oxford Network (VON) centres.21
Data collection
Retrospective descriptive datasets for this cohort study were linked for two decades from the labour ward register, neonatal admission register and presubmission data for the VON international benchmarking.21 Additional interrogation of the hospital inpatient enquiry system, labour ward weekly statistics for live and stillbirths, early pregnancy assessment unit (EPAU) statistics for early pregnancy loss/miscarriage information, inpatient ward statistics for early or late fetal loss during hospital admission as well as review of the hospital death certificate register were conducted to collate supportive information and to avoid ascertainment bias. We did not subclassify VLBW and ELBW births to spontaneous onset of labour with intact membranes, PPROM or medically initiated labour onset through induction or caesarean.7 Our VLBW and ELBW trends were compared with the published National figures from the Central Statistics Office (CSO) and National Perinatal Epidemiology Centre (NPEC) of Ireland.22 23
Region-wide search to collect data on home births during the lockdown and phase 1 and 2 of the easing of lockdown up to end of June 2020 was also conducted through community midwifery, ambulance centre and maternity emergency room database at UMHL.
Statistical analysis
Fully anonymised and deidentified dataset fulfilling general data protection regulation compliance was prepared for statistical analysis.24 Significance of temporal trends in the VLBW and ELBW rates per 1000 births were assessed using Poisson regression, where time was entered as a continuous variable. Poisson regression with 95% Wald CIs and rate ratio analysis were used to compare the observed VLBW rate for January to April of 2020 at UMHL to historical data. Estimates of the prevalence of VLBW and ELBW per 1000 births pre-2020 were assessed and the potential impact of January to April 2020 regional data on the national expectation of VLBW for 2020 in Ireland (based on the previous published Irish data from VON, NPEC and CSO).21–23 All data were analysed using IBM SPSS Statistics V.26.
Patient and public involvement
Patient and public involvement (PPI) was initiated at outset of research planning. Irish Neonatal Health Alliance (INHA), the patient advocacy group (Registered Charity Number: 20100100) representing parents of newborn infants in Ireland and member of European Foundation for the Care of Newborn Infants (EFCNI), was invited at the design stage of the study and was a signatory in the Research Ethics submission. INHA reviewed the aims of the study and confirmed that the issues addressed are of relevance to patients and public. INHA reaffirmed that the patient confidentiality is not breached at any stage, and specifically requested forecasting of National VLBW births through appropriate analysis in order for the advocacy group to prioritise family centred care programmes for 2020. INHA also nominated a parent of a premature VLBW infant as an independent external reviewer of VLBW and ELBW data for 2020. Designated representative of the patient advocacy group is a member of the study team and authorship of the manuscript. Once published, the relevant findings of the study will be disseminated through the websites of INHA www.inha.ie and EFCNI www.efcni.org. Guidance for Reporting Involvement of Patients and the Public reporting checklist as applicable to this study has been fulfilled (online supplemental table).
Supplemental material
Data verification and reporting
Considering the unprecedented and significant reduction of the VLBW and ELBW numbers observed during the lockdown and prelockdown phases of extra public health vigilance, we have verified the accuracy and authenticity of primary data capture with external independent professionals and patient representative (as part of the PPI initiative) who are not members of the research team or authorship. Such measures will minimise the ascertainment bias and underpins importance of data transparency.
Results
Over the last 20 years, UMHL had 93 018 live births and during the 4 months of January to April from 2001 to 2020 there were 30 705 live births. Annual live births, annual VLBW and ELBW rates as well as respective numbers for 1 January to 30 April of each year for the last two decades are summarised in table 1. Poisson regression analyses of the 2001–2019 data did not find any evidence of temporal trends for UMHL January to April VLBW (Wald χ2=0.784, p=0.376), January to April ELBW (Wald χ2=0.464, p=0.496), annual VLBW (Wald χ2=0.366, p=0.545) or annual ELBW (Wald χ2=0.008, p=0.929).
Regional data of VLBW and ELBW births for 2001–2020 from University Maternity Hospital Limerick, Ireland
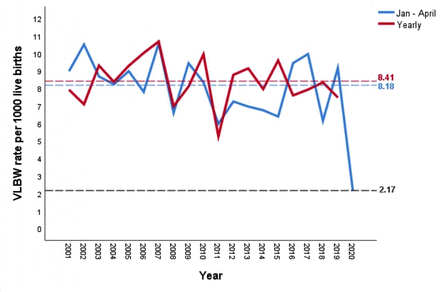
The VLBW rate per 1000 live births (January–April) based on aggregate 2001–2019 data was 8.18 (95% Wald CI 7.21 to 9.29), representing a forecast January–April 2020, in the absence of a temporal trend. However, the observed total number of only three VLBW in January–April 2020 (all of them born before mid-February 2020, with no ELBW) confirms an unusually low VLBW rate of just 2.17 per 1000 live births (95% Wald CI 0.70 to 6.74), 73% lower than the forecasted rate of 8.18 (figure 1).
VLBW births from January–April and Yearly for UMHL from 2001–2020. UMHL, University Maternity Hospital Limerick, Ireland; VLBW, very low birth weight.
The rate ratio comparing the risk of VLBW in January–April 2001–2019 to that from January to April in 2020 was 3.77 (95% Wald CI 1.21 to 11.75), p=0.022, suggesting that for two decades pre-2020 there was 3.77 times the rate of VLBW for the months of January–April in comparison to 2020. The ELBW rate per 1000 live births for January–April using aggregated data from 2001 to 2019 was 3.0 (95% Wald CI 2.43 to 3.70). There were no ELBW live births recorded for the health region during January–April 2020 (figure 2).
ELBW births from January–April and Yearly for UMHL from 2001–2020. ELBW, extremely low birth weight; UMHL, University Maternity Hospital Limerick, Ireland.
The VLBW rate per 1000 live births from the aggregated regional numbers for 2001–2019 yearly data was computed to be 8.41 (95% Wald CI 7.83 to 9.04), providing a forecasted annual rate for 2020. A continuation of the 73% reduction from the January–April VLBW rate for the health region for the remainder of 2020 would forecast a rate of 2.27 VLBW per 1000 live births. However, a reversal to the regional population’s prelockdown behavioural and socioenvironmental status quo could increase the rate towards historical rates.
The forecast for the 2020 national VLBW rate is taken from the 2014–2017 VON date for Ireland, giving a mean of 9.37 per 1000 live births; no trend is evident. If the national VLBW rate reflects the observed regional rate of 2.17 (95% Wald CI 0.70 to 6.74) (January–April 2020), the upper confidence limit estimates the number of VLBW infants to be born in Ireland in 2020 could be reduced to over 400 per 60 000 births (historically 500–600). (table 2) However, variation in the population’s compliance with lockdown, and postlockdown deterioration in behavioural and socioenvironmental factors or the possibility of a ‘baby boom’ in late 2020, could restore the historical VLBW rate of over 500 per 60 000 births.
National Irish data for VLBW and ELBW births based on the published CSO and VON numbers
Extended data surveillance from March to June 2020 confirmed that our initial observation sustained through the entire lockdown and phases 1 and 2 of the easing of restrictions, ELBW rate at 0.75 per 1000 live births (95% CI 0.11 to 5.36) and total VLBW (including ELBW) at 2.27 per 1000 (95% CI 0.73 to 7.03) (table 3). Mortality data analysis for March to June of 2016 to 2020 demonstrated no trends for ‘shift-to-left’ or ‘shift-to-right’ in 2020 (table 3), suggesting no evidence of early pregnancy loss, miscarriage or stillbirths being explanatory of the low rates of VLBW and ELBW in our region in Ireland. On the contrary, a trend towards a reduction in miscarriages was observed. LBW infants in the 1500–2000 g weight distribution also showed reduced births during this period in 2020 compared with previous years (table 3).
Early pregnancy loss, miscarriages, stillbirths, ELBW and VLBW births at University Maternity Hospital Limerick, Ireland, March–June 2016 to 2020 (data per 1000 live births)
There were no home deliveries of VLBW or ELBW infants during the lockdown in our region. Irish home birth rate is generally low and, in 2016, there were only 180 planned home births. Overall planned home birth rate in our health region in Ireland from September 2019 to June 2020 was only 15, at <0.05% of total births for the period.
Discussion
Prematurity poses significant medical, emotional, physical, psychological and financial burden for affected infants, their support network, health systems, economies and society as a whole.25 VLBW and ELBW infants may be affected by significant neonatal morbidity, leading to long-term health concerns during childhood.26 A myriad of aetiological and antecedent factors could trigger VLBW and ELBW births and the effectiveness of preventive measures depends on precise understanding of causation.10 A pan-European study found rising VLBW and ELBW rates in most countries.27 Increase in multiple births as well as assisted reproduction techniques (ART) also contributed to the overall increase.27 Even though earlier literature suggests PPROM as a multifactorial biological process, accounting for 30%–40% premature births, more recent medical interventions (indicated PTB) account for a significant proportion of VLBW infants.27–29 Understanding cross-country differences also could inform strategies aimed at reducing prematurity.17 27
Pregnancy is an ideal opportunity to encourage positive behavioural changes.30 Pregnancy Risk Assessment Monitoring System in Ireland, National Institute for Health and Care Excellence guidelines as well as the ‘Safer Maternity Care’ document in UK are worthy initiatives targeting reduced VLBW and ELBW births.30–32 Prenatal period and foetal growth could be regarded as a matrix for our lives and societies.33 Heterogeneous origins of VLBW and ELBW rates could be influenced by environmental changes, modifiable population factors, nutritional variations, stress factors and socioeconomic status.17 However, the yet under-recognised, behavioural, sociocultural and socioenvironmental modifications and opportunities designed to prolong the intrauterine nurturing milieu could offer far more in improving birth rates of such high-risk infants.
Birthweight-based data capture and analysis
Even though there has been increasing acceptance of GA-based cohorting,7 29 more recent neonatal network and register-based studies comparing VLBW and VLGA cohorts found no difference in the prediction power for adverse outcomes between the two groups despite the inherent SGA bias within the VLBW group.20 Two models also showed equal power to predict mortality and utility for benchmarking.20
The VON database and NPEC recorded 612 Irish infants in 2017 with gestation less than 29+6/7 weeks.21 23 Among this national cohort only 16 (2.6%) had a birth weight above 1500 g, indicative of VLBW being an acceptable proxy for significant prematurity.21–23 Contribution of SGA to the national VON submission in 2017 for VLBW was 19.5% and assuming a representative regional sample, our cohort of VLBW would have 80.5% premature infants who are appropriate for GA.21 23 These proportions could be significantly different in developing countries with relatively high SGA contribution among the VLBW infants.
Mortality trends: ‘shift-to-left’ and ‘shift-to-right’
Coinciding with the twenty year trend in VLBW and ELBW live births, we have also analysed the stillbirth rate (‘shift-to-right’) and compared with that of the lockdown period. Even though WHO defines stillbirth for fetal demise >28 weeks and Centers for Disease Control and Prevention defines >20 weeks; Irish CSO and Health Service Executive applies >24 weeks and that definition was applied to the study population.22 34 In order to establish that the decline in VLBW and ELBW rate during the lockdown was not secondary to an unexpected increase in early pregnancy loss (EPL <12+6/7 completed weeks of gestation) or terminations or miscarriages/late fetal loss (<24 weeks of gestation) (collectively ‘shift-to-left’), additional EPAU statistics and labour ward level data were collected for 2016–2020 for the months of March to June. As UMHL admits all infants with birth weight <2000 g to the neonatal unit, we also ascertained the trend of low birth weight (LBW <2.5 kg) infants of 1500–2000 g category for 2016–2019 and compared that with lockdown in 2020.
There was no increasing trend for EPL, miscarriages or stillbirths at UMHL or the region during the study period, confirming no ‘displacement of vital statistics’ due to ‘shift-to-left’ or ‘shift-to-right’ in mortality as the main explanation for the VLBW and ELBW reduction (table 3).
Potential influence of termination of pregnancy on VLBW and ELBW rates
As one of the few developed regions of the world with abortion legally banned till late 2018, Ireland offers a unique opportunity to evaluate the natural history of VLBW and ELBW births and the wider relation to socioenvironmental alterations.35 Could the ELBW and VLBW figures in early 2020 be explained partially by the change in termination of pregnancy (TOP) law, allowing for TOP beyond 12 weeks gestation in the presence of major congenital anomalies (MCA) that limits foetal or neonatal viability? Examination of our regional and national historical data suggest not.
Historical mean prevalence of MCA among our regional cohort of VLBW from 2000 to 2018 (two decades of no TOP) was 9.2% and the national means for 2014–2017 were 9%, 7%, 9% and 8%, respectively (55/596, 42/622, 54/593 and 51/612).23 That is, less than 1 in every 10 VLBW involved MCA when no TOP was available. The TOPs undertaken in 2019 and 2020 from January to April (two in 2019 and four in 2020) beyond 12 weeks of gestation in our region were for MCA, in accordance with the national guidelines on compassionate grounds.35
COVID-19 lockdown triggered socioenvironmental and behavioural modifiers
The ‘Nature’s experiment’ through the COVID-19 lockdown could have triggered unparalleled and widespread socioenvironmental alterations to which pregnant women would have responded with appropriate behavioural and lifestyle modifications. Our observational study is not designed to suggest causality or even association of specific factors or their particular influence exerted on the unprecedented reduction of VLBW rate from 8.18 (95% CI 7.21 to 9.29) to 2.17 (95% CI 0.70 to 6.74) per 1000 live births for the January to April period. Potential modifiers, both facilitators and barriers, in socioenvironmental settings that would have influenced the mother–fetus pair to reduce the rates of VLBW or ELBW births during the COVID-19 lockdown and prelockdown weeks of enhanced public health vigilance are summarised as a pictorogram (figure 3). Each one of the postulated reasons is supported by previous studies, often controlling or observing one or two variables. However, the COVID-19 lockdown possibly offered an unprecedented summative contribution of the socioenvironmental changes and behavioural modifications to impart a contemporaneous beneficial effect during pregnancy. An account of the previous studies favouring socioenvironmental and behavioural influence on VLBW and ELBW births is offered as an online supplemental file.
Supplemental material
COVID-19 lockdown in Ireland and reduction of birth of VLBW and ELBW infants: potential contributors. VLBW, very low birth weight; ELBW, extremely low birth weight.
COVID-19 lockdown triggered unfavourable social issues and access to care
It could be argued that that the lockdown impacted negatively on a subset of pregnant population due to imposed restrictions and constraints on timely access to hospital-based monitoring for fetomaternal well-being, possibly resulting in delayed or deferred interventions. It is plausible that such deferred choices could have contributed to the observed reduction in VLBW and ELBW rates. Pregnant women may have chosen to avoid hospital visits to mitigate potential for COVID-19 transmission. COVID-19 triggered changes in obstetric service provision, staff shortage, reduced number of ultrasound scans and screening, all may have impacted clinical interventions.36 However, the absence of concurrent or paired increase in EPL or miscarriages or stillbirths in our region, where the access to maternity emergency services were functioning uninterrupted throughout the lockdown, supports non-medical and societal contributions to observed significant reduction in the VLBW and ELBW numbers.
Learning from the lockdown and societal approaches to influence VLBW rates
Only three VLBW and no ELBW infant admissions to the only neonatal intensive care unit of one of the health regions of Ireland from 1 January to 30 April 2020, resulted in a reduction to zero of morbidity metrics primarily linked to extreme prematurity such as necrotising enterocolitis, retinopathy of prematurity and severe forms (grades 3 and 4) of intraventricular haemorrhage. While the generalisation of the morbidity reduction is limited by the small regional sample, our findings highlights the prevention of ELBW births, if not absolutely medically indicated, as an effective approach in improving the high-risk and high-cost complications associated with extreme prematurity.
Broadened preventive approaches based on socio-environmental alterations, stress reduction, nutritional optimisation and lifestyle modifications based on underlying individual genetic and epigenetic variations may be worth considering.25 These observations, if replicated in other regions globally during the pandemic and linked with varying levels of socio-environmental restrictions triggered by COVID-19, could offer novel perspectives and promising insights facilitating analysis of yet under-appreciated phenotypes of VLBW and ELBW births. Statistical modelling approaches and big-data analysis principles would also be critical.16
Our observed trend in VLBW and ELBW births, if an outcome of the COVID-19 enforced socioenvironmental and behavioural changes, suggest it is reasonable to postulate that, (1) the low numbers from early March onwards was influenced by the effects of the prelockdown period of extra public health vigilance that commenced in mid-February, (2) effects are immediate and (3) the effects of lockdown will be seen in coming months and sustainable until such time as normality influencers are operating again. However, postlockdown deterioration in socio-environmental factors or a ‘baby boom’ in late 2020 could increase the VLBW and ELBW rates.
With limited international data published to date, emerging report from Denmark suggested a nationwide reduction of extremely premature births in the order of 90% during COVID-19 lockdown, compared with the preceding 5 years.37 A quasi-experimental study from Netherlands is suggesting reduction in PTB of all strata during the various time windows of the lockdown, compared with the preceding ten years.38 Newspapers, television and radio broadcasters as well as social media outlets from around the world during the last 2 months also report the possibility of an unexpected variation in the very preterm and VLBW/ELBW rates from diverse regions where a COVID-19 lockdown was imposed.39–41 However, reports of status quo or even an increase in VLBW rates from certain cities and increase in stillbirth rate36 also raise the possibility that it is perhaps how pregnant women respond to the cumulative socioenvironmental alterations and what level of medical, social, familial and economic support systems are offered in different countries or regions during the lockdown that influences the fetomaternal outcome.
Limitations, interpretations and generalisability
The following limitations are acknowledged: (1) Inherent reservations posed by retrospective nature of the birth cohort data spanning over two decades from one health region of Ireland; (2) Even though the vast majority of the VLBW infants would be premature, concurrent contribution by SGA and rarely severe IUGR at term could be included. However, such an inclusion consistently over two decades should reduce the bias and the weight-based inclusion criteria would allow comparison to national data by CSO, NPEC and internationally through VON; (3) Inclusion of January 2020, when there was no lockdown or enhanced prelockdown public health measures. This was required to make comparison with the two decades of trends including the ‘first four calendar months’; (4) Completion of the study prior to the official finish of lockdown was to facilitate ease of comparison against the coded historical monthly data, timely data completion and analysis. However, we have extended our observation through the entire lockdown and the phase 1 and phase 2 of the easing as well (till end of June 2020) and confirmed that our initial observation sustained; (5) ELBW cohort could only be analysed with limitations considering the small number of births; (6) We caution the ‘no abortion policy’ that Ireland followed till late 2018, when making international comparisons; (7) The lockdown could have deferred what should have been medically offered early during pregnancy, thus arguably postponing the GA of intervention. Thus, it could be viewed that the potential for reduced monitoring opportunities or the deferred early foetomaternal interventions during the lockdown could have also ‘shifted the band’ from ELBW and VLBW to LBW or normal weight and gestational category of infants; (8) Our observations could either be due to the cumulative socio-environmental alterations and maternal behavioural modifications or due to deferred early obstetric interventions or suboptimal timely access to the recommended antenatal monitoring. Our study is not designed to confirm causality or reaffirm associations and the postulated factors summarised in figure 3 and online supplemental file reflects compilation of already existing evidence; (9) Dataset from a regional sample in Ireland is relatively small and thus not strictly reflecting every society’s behavioural and socioenvironmental response to the country-specific components of COVID-19 lockdown and the offered support systems.
Conclusion
The Irish national lockdown in response to SARS-CoV-2 virus (COVID-19) pandemic and the cumulative effects of socioenvironmental variables such as maternal behavioural modifications, opportunities to WFH, potential reduction in work related stresses, possible alleviation of physical strain related to work and commuting, optimal opportunities for rest and sleep, likely increase in partner presence and support at home, reduced exposure to infections, improved opportunities for nutritional support and exercise as well as the positive alterations in environment and air pollution, all could have possibly contributed to the reduction in births involving VLBW and ELBW infants. Potential contribution of deferred early obstetric interventions or suboptimal access to recommended antenatal monitoring, either due to institutional or patient level COVID-19-related concerns, shifting the birth weight spectrum also remains a possibility. Further research is needed to enhance our knowledge regarding the complex ways in which environmental, social, behavioural and biological factors interact and modify the VLBW and ELBW births. We recommend that WHO and national policy-makers reflect on this positive outcome of the COVID-19 pandemic, the insight that it has provided, and seize the opportunity to support further studies from geographically diverse regions evaluating implicated interdependent behavioural and socioenvironmental modifiers that may potentially influence VLBW and ELBW births.
Acknowledgments
Authors wish to acknowledge Thomas Stack, Gerard Burke, Con Sreenan, Niazy Al-Assaf, Margo Dunworth, Deirdre O’Connell, Marie Carroll, Collette Quinn, Irene Beirne, Brenda Hayes, Leona Blackwell and Eamon Leahy for various stages of neonatal and perinatal activity tabulation and verification over the two decades at UMHL. Athanasios Mantas is acknowledged for the information related to the termination of pregnancy (TOP) and Grace McCormack for collating the labour ward activity at UMHL. John Slevin and Rizwan Khan (obstetric and neonatal professionals) as well as Sharon O’Brien (parent of a VLBW infant, as part of PPI) are appreciated for their independent scrutiny and verification of primary VLBW and ELBW data for 2020. Patrick Dillon and Joanne O’Connor are acknowledged for the research governance and ethics approvals. Noreen Mann and Angela O’Farrell from M3 ward and Jean Rafferty from the early pregnancy assessment unit (EPAU) for collating the early pregnancy loss, miscarriages and stillbirth data. National Perinatal Epidemiology Centre (NPEC) is acknowledged for the recent Vermont Oxford Network (VON) Ireland information and the Central Statistics Office (CSO) of Ireland for the National data. Obstetric, midwifery, nursing and neonatal professionals of UMHL who otherwise supported the project through their clinical input and assistance are gracefully acknowledged.
References
Footnotes
Handling editor Sanni Yaya
Twitter @roykphilip
Contributors RKP conceptualised and designed the study, extracted the VLBW and ELBW data, drafted the initial draft, reviewed and revised the manuscript. ER collected the neonatal activity data and contributed to the nursing and midwifery sections. HP developed the data analysis instruments, conducted the statistical analysis and reviewed and revised the relevant sections. MI contributed to the obstetric data, verified the termination of pregnancy register and reviewed the relevant sections. MD contributed as the patient and public representative, contributed to the relevant sections and developed the search strings. NHO co-supervised the research and critically reviewed the infection and microbiology sections. DM cosupervised the research, reviewed and edited the relevant sections. CPD coordinated and supervised the research, advised on methodology and manuscript structure and critically reviewed the manuscript for important intellectual content. All authors approved the final manuscript as submitted and agree to be accountable for the work. The corresponding author attests that all listed authors meet authorship criteria and that no others meeting the criteria have been omitted.
Funding The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors.
Disclaimer The views expressed are those of the authors and not necessarily those of employing authorities of authors such as Health Service Executive (HSE), University of Limerick or Irish Neonatal Health Alliance (INHA).
Competing interests None declared.
Patient and public involvement Patients and/or the public were involved in the design, or conduct, or reporting, or dissemination plans of this research. Refer to the Methods section for further details.
Patient consent for publication Not required.
Ethics approval University Hospital Limerick Research Ethics Committee approval was granted for the study (No: 048/2020 dated 6 May 2020).
Provenance and peer review Not commissioned; externally peer reviewed.
Data availability statement All data relevant to the study are included in the article or uploaded as online supplemental information.