Article Text
Abstract
Introduction Human papillomavirus (HPV) self-sampling test kits may increase screening for and early detection of cervical cancer and reduce its burden globally. To inform WHO self-care guidelines, we conducted a systematic review and meta-analysis of HPV self-sampling among adult women on cervical (pre-)cancer screening uptake, screening frequency, social harms/adverse events and linkage to clinical assessment/treatment.
Methods The included studies compared women using cervical cancer screening services with HPV self-sampling with women using standard of care, measured at least one outcome, and were published in a peer-reviewed journal. We searched PubMed, the Cumulative Index to Nursing and Allied Health Literature (CNIAHL), Latin American and Caribbean Health Sciences Literature (LILACS) and Embase through October 2018. Risk of bias was assessed using the Cochrane tool for randomised controlled trials (RCTs) and the Evidence Project tool for non-randomised studies. Meta-analysis was conducted using random-effects models to generate pooled estimates of relative risk (RR).
Results 33 studies in 34 articles with 369 017 total participants met the inclusion criteria: 29 RCTs and 4 observational studies. All studies examined HPV self-sampling; comparison groups were standard of care (eg, Pap smear, visual inspection with acetic acid, clinician-collected HPV testing). 93% of participants were from high-income countries. All 33 studies measured cervical cancer screening uptake. Meta-analysis found greater screening uptake among HPV self-sampling participants compared with control (RR: 2.13, 95% CI 1.89 to 2.40). Effect size varied by HPV test kit dissemination method, whether mailed directly to home (RR: 2.27, 95% CI 1.89 to 2.71), offered door-to-door (RR: 2.37, 95% CI 1.12 to 5.03) or requested on demand (RR: 1.28, 95% CI 0.90 to 1.82). Meta-analysis showed no statistically significant difference in linkage to clinical assessment/treatment between arms (RR: 1.12, 95% CI 0.80 to 1.57). No studies measured screening frequency or social harms/adverse events.
Conclusion A growing evidence base, mainly from high-income countries and with significant heterogeneity, suggests HPV self-sampling can increase cervical cancer screening uptake compared with standard of care, with a marginal effect on linkage to clinical assessment/treatment.
Systematic review registration number PROSPERO CRD42018114871.
- human papillomavirus
- cervical cancer screening
- self-sampling
- systematic review
- meta-analysis
This is an Open Access article distributed under the terms of the Creative Commons Attribution IGO License (https://creativecommons.org/licenses/by-nc/3.0/igo/), which permits use, distribution, and reproduction for non-commercial purposes in any medium, provided the original work is properly cited.
Statistics from Altmetric.com
Key questions
What is already known?
Cervical cancer is one of the most common types of cancer among women globally and the leading cause of cancer deaths in women in low-income and middle-income countries, but early detection and treatment of precancerous lesions can prevent cervical cancer.
High-risk human papillomavirus (HPV) testing is a relatively new, reasonably accurate method of secondary cervical cancer prevention.
What are the new findings?
Meta-analysis shows that self-sampling for HPV testing may increase population uptake of cervical cancer screening, especially when HPV self-sampling kits were sent directly to women’s homes or offered door-to-door by a health worker.
However, linkage to follow-up testing and treatment after HPV self-sampling and after regular screening services alike is limited.
What do the new findings imply?
A WHO recommendation on self-sampling for HPV may increase screening coverage (although strategies for improving linkage to treatment after positive test results are needed) and decrease the burden of cervical cancer.
Introduction
Cervical cancer is one of the most common types of cancer among women globally; in low-income and middle-income countries (LMICs), it is the leading cause of cancer deaths in women.1 2 Cervical cancer develops from persistent high-risk human papillomavirus (HPV) infection.3 Although vaccines exist that protect against infection and disease associated with specific types of HPV, many women in LMICs do not have access to HPV immunisation and die of this preventable cancer.3 Secondary prevention measures include early detection and treatment of precancerous lesions. Cervical cancer screening has successfully reduced cervical cancer incidence and mortality, especially in high-income settings with effective population-based screening programmes with good organisation, coverage and quality.4 5 In organised screening programmes, the majority of new cases are found in women who are never screened or underscreened; these women are often diagnosed at a later or more advanced-stage cancer, requiring more invasive treatment and leading to lower quality of life and survival.6 However, screening programmes require that a cervical cancer screening test—such as cervical cytology (Pap smear), visual inspection with acetic acid (VIA) or HPV testing—is available and accessible.
Unfortunately, in many countries, standard cervical cancer screening tests are not universally or even widely available: although almost 81% of countries have cervical cancer policies and strategies, only 48% have an operational plan with funding.7 The magnitude of this public health problem necessitates innovative approaches to support women, families and communities. Reaching more at-risk women with HPV testing, including women living with HIV who have higher risk of HPV infection and cervical cancer, is critical.8 Additionally, the two-decade to four-decade lag time between the peak of HPV infection and the peak of cervical cancer incidence leaves great opportunity for prevention.3 Primary high-risk HPV testing is a relatively new method of secondary cervical cancer prevention.9–12 A 2018 review found that, compared with clinician samples, self-collected HPV samples showed reasonably high diagnostic accuracy, although assays based on PCR showed better performance than those based on signal amplification.12 HPV testing through self-collected specimens has gained attention for its potential to increase screening participation. Self-sampling requires individuals to obtain a kit, collect their own samples and send their specimens to a laboratory; the laboratory tests the self-collected specimens and returns the test result to the individual.13 Self-sampling can be conducted either at the clinic or outside the health system and can be initiated either by health providers or by the clients themselves. Accountability of and linkage to the health sector are important considerations for the success of this self-care intervention, including providing quality test kits, recollecting kits equitably and ensuring follow-up after self-sampling kit usage. Four systematic reviews of randomised trials in the context of population-based screening programmes showed that offering high-risk HPV self-sampling to never-screened and underscreened women increased participation compared with inviting women to have samples taken by health professionals.12 14–16
In order to develop normative guidance by the WHO on self-care interventions for sexual and reproductive health and rights, we conducted a systematic review of available evidence on the effectiveness of HPV self-sampling on increasing uptake and frequency of cervical cancer screening, social harms/adverse events, and linkage to care after a positive screening result.
Methods
We conducted this systematic review in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines.17 A full protocol is available on the PROSPERO database.
Definition
HPV self-sampling is a process where a woman who wants to know whether she has HPV infection uses a kit to collect a (cervico-)vaginal sample, which is then sent for analysis by a laboratory. Collection methods include lavage, brush, swab and vaginal patch. While HPV self-sampling cannot provide a diagnosis of cervical (pre-)cancer, it identifies those women at higher risk. The privacy afforded by self-sampling may encourage more people to get tested compared with Pap smears that, especially in LMICs, still have low coverage due to limited population awareness and lack of availability.
Research question and inclusion criteria
This review addressed the following research question: Should HPV self-sampling be offered as an additional approach to clinician-based sampling and cervical cancer screening services, including cervical screening by cytology (Pap smears) or VIA testing services?
Population
Women aged 30–60.
Intervention
Cervical screening services that include HPV self-sampling.
Comparison
Cervical screening services that do not include HPV self-sampling (eg, cervical screening by cytology, VIA testing services, clinician-collected primary HPV testing).
Outcomes
Uptake of cervical cancer screening services (ie, population coverage, or proportion of those offered HPV testing or other screening methods who accepted and completed screening);
Frequency of cervical cancer screening (ie, frequency of self-sampling compared with frequency of standard of care);
Social harms/adverse events (eg, device-related issues, coercion, violence (including intimate partner violence, violence from family members or community members and so on), psychosocial harm, self-harm, suicide, stigma, discrimination, frequency of testing for sexually transmitted infections and HIV) and whether these harms were corrected/had redress available; and
Linkage to clinical assessment or treatment of cervical lesions following a positive self-test result and positive diagnosis for HPV by a healthcare provider (ie, among people who have a positive test result, the percentage who reach this next stage of management).
To be included in the review, an article had to (1) have a comparative study design examining women who received HPV self-sampling services with women who received HPV testing services through another modality, or to another screening test or to no intervention (ie, no cervical cancer screening services); (2) evaluate one or more of the outcomes listed above; and (3) be published in a peer-reviewed journal.
Inclusion was not restricted by location of the intervention. No language or publication date restrictions were used in the search.
Search strategy and screening process
We searched the electronic databases PubMed, the Cumulative Index to Nursing and Allied Health Literature (CINAHL), Latin American and Caribbean Health Sciences Literature (LILACS) and Embase through 19 October 2018 using search terms for HPV and self-sampling. The full search strategy is available in online supplementary file 1. Secondary reference searching was also conducted on all studies included in the review and on four relevant systematic reviews.12 14–16 Ongoing randomised controlled trials (RCTs) were searched for through ClinicalTrials.gov, the WHO International Clinical Trials Registry Platform, the Pan African Clinical Trials Registry and the Australian New Zealand Clinical Trials Registry.
Supplemental material
After initial title–abstract screening, full-text articles were obtained of all potential studies. Two reviewers independently assessed all full-text articles for study inclusion eligibility and resolved differences through consensus.
Data extraction and analysis
Two reviewers independently extracted data and conducted the quality assessments. Standardised data extraction forms included fields for study citation, objectives, location, population characteristics, description of the type of HPV sampling, description of any additional intervention components, study design, sample size, follow-up periods and loss to follow-up, analytic approach, reported numerical outcomes, results, and limitations.
For RCTs, risk of bias was assessed using the Cochrane Collaboration’s tool for assessing risk of bias.18 For observational studies that presented comparative data, study rigour was assessed using the Evidence Project risk of bias tool for intervention evaluations.19
Where available, comparative data were stratified by the following categories: supervised (defined as direct support through inperson demonstration of how to perform self-sampling and follow-up support, counselling, referral and linkage to care) versus unsupervised (defined as indirect support through video, instructions for use, package inserts, hotline, or other information which provides counselling, support, referral and linkage to care); age (<50 vs ≥50 years); vulnerabilities (relating to poverty, disability, living with HIV, sex work or literacy); and high-income versus low-income or middle-income countries.
Data were analysed according to coding categories and outcomes. Where multiple studies reported the same outcome, we conducted meta-analysis using random-effects models to generate pooled relative risk (RR) using the Comprehensive Meta-Analysis program.20 Where studies reported both intention-to-treat and per-protocol analyses, we used intention-to-treat data. Where studies reported multiple follow-up periods, we used the longest follow-up time. Heterogeneity was assessed using both Q and I-squared statistics, and funnel plots were created to examine the potential for publication bias. Data from RCTs and non-randomised studies were analysed separately.
For the uptake of cervical cancer screening outcome, we combined authors’ reported data on screening participation, attendance, response and compliance. Where studies reported uptake for conventional cytology (Pap smears), VIA or clinician-collected HPV testing in addition to HPV self-sampling, we combined uptake of any cervical cancer screening method reported among the HPV self-sampling group. Where more than one control group was reported, we compared the intervention group with the least intensive sampling strategy control group.
Patient and public involvement
A representative from a community of women living with HIV in India reviewed the manuscript for readability and accuracy and offered discussion points. Patients are currently involved in a global survey of values and preferences and focus group discussions with vulnerable communities, conducted to inform the WHO self-care guideline; they thus play a significant role in the overall recommendation outcome from this review.
Results
Electronic database searching retrieved 1847 citations. Searching trial registries, contacting experts in the field and secondary searching identified an additional 11 citations (figure 1). After removing duplicates, there were 1099 unique citations. After initial screening of titles and abstracts, 361 citations remained. After two independent reviewers screened in duplicate and gained consensus, 149 articles were pulled for full-text review. Of these, 33 studies (reported in 34 articles) were included in the review.21–54
PRISMA flow diagram of the different phases of a systematic review. PRISMA, Preferred Reporting Items for Systematic Reviews and Meta-Analyses.
Study characteristics
Table 1 presents summary characteristics of the 34 included articles. The 33 studies included 369 017 total participants; individual study sample sizes ranged from 63 to 36 390. Articles were published between 2007 and 2018; two-thirds were published in the last 4 years. Studies were primarily conducted in high-income countries (one article each in Argentina, Australia, Belgium, Slovenia and Switzerland; two in England, Finland and Italy; three in Canada, Denmark, France and the Netherlands; four in Sweden and the USA). One study each took place in Mexico, Nigeria and Uganda. Of the included women, 93% were from high-income countries. Studies occurred in urban (n=14), mixed urban/rural (n=15) and rural settings (n=5).
Description of included studies and reported outcomes
All studies included a study arm where women used cervical cancer screening services with HPV self-sampling (cervicovaginal sampling devices included 15 brush, 12 swab, 6 lavage and 3 not reported) and a control group with standard of care (eg, standard reminder letters/recommendation to get screened, Pap smears/conventional cytology, VIA or clinician-collected HPV testing). Most studies implemented opt-out HPV self-sampling by sending an HPV self-test kit directly to participants’ home addresses (n=24). Six studies used opt-out HPV self-sampling offered door-to-door by a health worker (either a nurse, community health worker or research staff). Seven studies had participants opt in to HPV self-sampling by requesting a test kit by phone, mail, text message or website, or by picking up a test kit from a local pharmacy or health centre. In one study, participants self-collected samples for HPV testing in an HIV clinic.
Study participants typically comprised adult women from the general population, most often non-respondents in routine population-based cervical cancer screening programmes. Five studies were conducted among immigrant women, ethnic minorities and women from medically underserved/low socioeconomic status regions. One study each took place among women from First Nations communities and women living with HIV. Participants’ ages ranged from 18 to 70, but participants were most often between 30 and 60 years old. All studies measured uptake of cervical cancer screening, but follow-up periods ranged from immediately after being offered screening to 36 months, with half between 6 and 12 months.
Study designs included 29 RCTs and 4 observational studies (3 prospective cohort studies and 1 cross-sectional study). Risk of bias in RCTs was generally low. Although it was impossible to blind participants and personnel to HPV self-sampling versus standard of care, we judged most outcomes were not likely to be influenced by lack of blinding. The observational studies were of moderate quality. Table 2 (for RCTs) and table 3 (for non-RCTs) present an assessment of study rigour. The Grading of Recommendations Assessment, Development and Evaluation (GRADE) table for this review with quality assessment by outcome is available in online supplementary file 2.
Supplemental material
Quality assessment of included studies (RCTs)
Quality assessment of included studies (non-RCTs)
For each of the main outcomes, the results are presented below and summarised in table 4.
Summary of effect sizes and meta-analyses
Uptake of cervical cancer screening services
All 34 included articles reported some measure of uptake of cervical cancer screening. Substantial heterogeneity was present in all meta-analyses of screening uptake. Combining all self-sampling kit dissemination methods, meta-analysis of the 29 reported effect sizes from RCTs21–25 27 29–36 38–47 50–54 found that women were twice as likely to use cervical cancer screening services through self-sampling compared with standard-of-care screening practices (RR: 2.13, 95% CI 1.89 to 2.40, I-squared: 99.34) (figure 2).
Meta-analysis showing relative risk of uptake of cervical cancer screening, overall.
Uptake stratified by HPV self-sampling kit dissemination strategy
In the 23 RCTs comparing opt-out HPV self-sampling (kit directly mailed to home address) with control,22–24 27 29–36 39 42 43 45–47 51–54 meta-analysis found that HPV self-sampling was associated with twice the likelihood of attending screening compared with control (RR: 2.27, 95% CI 1.89 to 2.71, I-squared: 99.27) (figure 3). These RCTs all took place in Europe, except for two in Canada and one in Nigeria. RCT participants were all non-respondents to regular screening, except for one RCT among general population women and one among First Nations communities. All intervention arm participants self-sampled outside the clinic (ie, at home or work) without supervision using a variety of sampling kit types. One observational study showed a similar effect. In Finland, a prospective cohort study followed 31 053 women identified for regular cervical cancer screening.49 A second reminder letter after initial invitation increased screening participation from 72.6% to 79.2% (95% CI 78.8 to 79.7), and sending a self-sampling test kit directly to women’s home further increased overall uptake to 82.2% (95% CI 81.8 to 82.7).
Meta-analysis showing relative risk of uptake of cervical cancer screening, opt-out (self-sampling kit directly mailed to home) versus control.
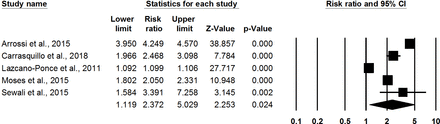
Six studies compared opt-out HPV self-sampling offered door-to-door by health workers with control.21 25 26 38 40 44 In these studies, a community health worker, nurse or health outreach worker would visit participants’ homes, provide education on cervical cancer and screening, offer a self-sampling HPV test kit (brush or swab) to the participant, and collect the kit for lab testing. Meta-analysis of five RCTs21 25 38 40 44 showed that women were almost three times as likely to participate in cervical cancer screening (RR: 2.37, 95% CI 1.12 to 5.03, I-squared: 99.72) (figure 4). Two of these RCTs took place in the USA among ethnic minority or immigrant women, one each took place in Argentina and Uganda among women in the general population, and one took place among medically underserved women from a poverty reduction programme in Mexico. One prospective cohort study on community outreach in the rural Mississippi Delta, USA, found that medically underserved non-respondents to the regular screening programme responded more to an offer of the HPV self-sampling kit and cervical cancer education (62/77, 80.5%) than to a voucher for a free Pap test with staff-facilitated appointment scheduling at the local clinic (17/42, 40.5%).26
Meta-analysis showing relative risk of uptake of cervical cancer screening, opt-out (self-sampling kit offered door-to-door by health worker) versus control.
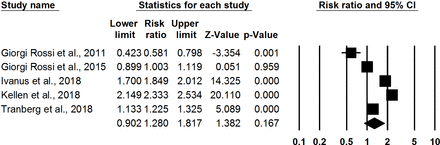
Meta-analysis of five RCTs29 30 35 36 47 found a non-significant increase in likelihood of HPV screening participation for opt-in HPV self-sampling where participants requested or picked up self-sampling kits compared with control (RR: 1.28, 95% CI 0.90 to 1.82, I-squared: 98.36) (figure 5). These RCTs all took place in Europe among women aged 30–65 who were hard to reach through conventional cervical cancer screening programmes. Women could order HPV self-sampling kits by email, text message, phone, website or mail; kits could be delivered to participants’ homes or picked up at a local pharmacy or health centre. All participants in the intervention arm self-sampled at home without supervision. Two observational studies presented similar increases in uptake. In Denmark, the Copenhagen Self-Sampling Initiative invited women to opt in to order a HPV self-sampling kit by mail, phone, email or website.37 Of 23 632 women invited, 7484 women ordered a self-sampling brush and 4824 returned the brush for DNA testing; 2288 received screening by a physician. A 2-year prospective cohort study in Canada compared preintervention and postintervention screening rates in three communities: HPV self-test and cervical cancer education/promotion campaign, campaign alone and no intervention.28 In the community receiving self-test kits and the campaign, the cervical cancer screening rate increased by 15.2% (p<0.001), compared with the campaign alone (+2.9%, p=0.07) and no intervention (+8.5%, p<0.001).
Meta-analysis showing relative risk of uptake of cervical cancer screening, opt-in (self-sampling kit on demand) versus control.
One RCT in Baltimore, Maryland, USA, examined the impact of HPV self-sampling among women living with HIV.41 Women who self-collected cervicovaginal specimens for HPV testing in the HIV clinic were not more likely to complete cytology within 6 months compared with women who received only a reminder to make a cervical cancer screening appointment (22/63 vs 12/31, two-group test of proportions, p=0.59, RR: 0.93, 95% CI 0.51 to 1.69).
Uptake stratified by setting
Of the 29 included RCTs, 26 took place in high-income countries21–25 27 29–36 41–47 50–54 and 3 in LMICs38–40 as classified by the World Bank. In meta-analysis, HPV self-sampling was associated with increased uptake in both economic classifications, with greater impact in high-income countries (RR: 2.24, 95% CI 1.86 to 2.71, I-squared: 99.38) than in LMICs (RR: 1.54, 95% CI 1.01 to 2.34, I-squared: 98.43). Similarly, meta-analysis found increased uptake among HPV self-samplers regardless of setting, although potentially stronger effects were seen in urban areas (RR: 2.07, 95% CI 1.54 to 2.83, I-squared: 99.21)22 31 32 39–46 48 50 51 and mixed urban/rural areas (RR: 1.96, 95% CI 1.45 to 2.65, I-squared: 99.28)21 23–25 27 29 30 33–36 45 48 than in rural settings (RR: 1.40, 95% CI 1.14 to 1.73, I-squared: 89.69).38 45 48 53 54
Uptake stratified by sociodemographics
Twelve RCTs were conducted solely among (or included disaggregated data for) women under 50 years of age23 24 29 33 34 36 38 39 42 43 45–47 50 and 11 RCTs among women over 50.23 24 29 34 36 38 39 42 43 45–47 50 In meta-analysis, HPV self-sampling showed a slightly stronger impact on uptake among older women (RR: 2.25, 95% CI 1.44 to 3.50, I-squared: 99.18) than among younger women (RR: 1.95, 95% CI 1.61 to 2.36, I-squared: 99.04). Four RCTs presented data for low socioeconomic status women24 38 39 47 and three for high socioeconomic status women.24 39 47 Meta-analysis found increased uptake after HPV self-sampling compared with standard-of-care cervical cancer screening, both among low socioeconomic status women (RR: 1.62, 95% CI 1.15 to 2.28, I-squared: 96.24) and high (RR: 1.40, 95% CI 1.15 to 1.71, I-squared: 27.65).
Uptake stratified by supervision
Two of the 29 included RCTs had participants self-collect samples for HPV testing under supervision; one used community health worker support for Hispanic, black and Haitian women self-sampling in Miami-Dade, Florida, USA,25 while the other used nurse support for women self-sampling in a poverty reduction programme in rural Mexico who had limited access to health services.38 Meta-analysis found greater uptake among supervised self-samplers (RR: 2.21, 95% CI 1.80 to 2.73, I-squared: 99.10)25 38 than among women self-sampling for HPV testing without supervision (RR: 1.63, 95% CI 0.74 to 3.61, I-squared: 97.94).21–24 27 29–36 39–47 50–54
Frequency of cervical cancer screening
None of the included articles reported comparative data on frequency of cervical cancer screening.
Social harms and adverse events
None of the included articles compared outcomes relating to social harms and adverse events between HPV self-sampling and other cervical cancer screening services.
Linkage to clinical assessment or treatment of cervical lesions
Six of the included articles—five RCTs conducted among women who were not responding to standard screening programme algorithms in high-income settings in Europe who were mailed HPV self-sampling kits and one RCT offering HPV self-sampling door-to-door in Uganda—reported on linkage to clinical assessment or treatment of cervical lesions following a reactive self-test result and/or positive diagnosis for HPV by a healthcare provider.24 29 33 40 43 51 Meta-analysis found no difference in the rate of postscreening linkage to care among women who received a positive screening result between arms (RR: 1.12, 95% CI 0.80 to 1.57, I-squared: 84.16) (figure 6). The study in a low-income country had potentially lower linkage to follow-up care (RR: 0.66, 95% CI 0.43 to 1.00)40 compared with high-income countries (RR: 0.94, 95% CI 0.78 to 1.14, I-squared: 86.03),24 29 33 43 51 although no appreciable difference was discerned in either setting nor either kit dissemination method.
Meta-analysis showing relative risk of linkage to clinical assessment or treatment, self-sampling versus control.
Discussion
Cervical cancer control is an essential priority for the WHO and many other partners. Available and accepted screening methods (ie, cytology, VIA or clinician-collected HPV testing) to detect women at risk for (pre-)cancer are not practical or accessible to the majority of women living in low-resource settings. Alternative screening strategies that decrease structural and other access challenges faced by women include self-sampling for HPV, as it is a simple intervention that women can use which supports their right to health. It also grants privacy and convenience to women, bypassing common barriers like fear, shame, geographical barriers, time limitations, cultural or religious considerations, and lack of access.55 Self-sampling has the potential to overcome the practical and personal barriers which may prevent some women from responding to standard cervical cancer screening.
Although interstudy heterogeneity was observed, the existing literature generally suggests that using HPV self-sampling methods, especially opt-out methods, increases uptake of cervical cancer screening services. When self-sampling kits were mailed directly to women’s home addresses, meta-analysis of 22 RCTs showed that likelihood of attendance in the self-sampling arm was twice as high as the control. Data from observational studies corroborated these findings. Comparison of different strategies showed greater impact with HPV self-sampling offered door-to-door by health workers than by mailing kits directly to homes and by giving participants the responsibility to request or pick up kits, but the generally wide CIs around these estimates limit our ability to say for sure. Interestingly, in both opt-out strategies (mailed directly home and offered door-to-door), all effect sizes suggested that HPV self-sampling increased participation despite significant heterogeneity; when participants were given the choice to opt in to HPV self-sampling, the uptake outcome included mixed positive and negative effects. Quantitative heterogeneity in meta-analyses may be partially attributable to the use of RR for percentages instead of rates across studies, since high participation in control groups shifts the RR closer to 1.
No studies offered comparative data for frequency of cervical cancer screening, nor for social harms and adverse events. Given that cervical cancer screening is recommended at relatively infrequent intervals, often up to 5 years, it is understandable that studies generally did not assess this longer term outcome. One follow-up study to an included RCT found that, on regular invitation to subsequent clinic-based cervical cancer screening 3 years after invitation to an HPV self-sampling trial, there was no statistically significant difference in participation rate (approximately 30% in all arms) comparing those randomised to HPV self-sampling with HPV testing in clinic, whether prior self-sampling was conducted at home (RR: 1.05, 95% CI 0.90 to 1.22) or at a pharmacy (RR: 0.96, 95% CI 0.83 to 1.22).56 However, although the initial RCT compared self-sampling (sent kit home or offered free at local pharmacy) with standard population-based screening (sent reminder for cervical specimen taken at clinic), all women at the 3-year follow-up timepoint were reinvited for clinic-based HPV screening.
Finally, limited findings suggest that HPV self-sampling results in similar rates of linkage to clinical assessment or treatment of cervical lesions compared with standard services. No difference in linkage to follow-up diagnosis or treatment was found, regardless of kit dissemination method. Interestingly, compliance to follow-up testing and treatment was low in settings like France,43 where cervical screening programmes do not actively propose ascertainment appointments (eg, triage cytology, colposcopy) after positive initial screening results, but was relatively high in settings with organised programmes including active follow-up like England,24 Italy29 and Sweden.33 While it is encouraging that linkage to care was not decreased among self-samplers, the generally low rate of clinical follow-up after a positive screening result is a cause for concern.
Strengths and limitations
This study had several strengths. We included both randomised and non-randomised studies, searched multiple databases, considered studies in any location or language, and used meta-analysis to present pooled effect sizes. Other reviews have examined the impact of HPV self-sampling on screening participation among women who are never or infrequently attending cervical cancer screening services, reporting that self-sampling has great potential to increase attendance among underscreened women compared with invitations to have a Pap test done by a health professional.12 14–16 This review expands on previous work by incorporating evidence from general populations and other segments of the population, finding similar increases in uptake overall, not just among non-responders.
Our confidence in the findings is strengthened by the large number of rigorously conducted studies identified. However, despite identifying 34 articles which met our inclusion criteria, almost all of the included studies took place in high-income countries, where population-based cervical cancer screening programmes are more common. Additional research is needed to expand the evidence base in LMICs.
Further research should seek to answer questions surrounding how HPV self-sampling will be experienced by users in different settings and in different social and relationship contexts. For example, screening programmes may differ by the support available for self-sampling, mechanisms for test kit distribution and return, and linkages to diagnostic testing and subsequent triage to treatment. A systematic review of non-comparative or qualitative studies exploring users’ experiences of self-sampling and impact on discrimination or other social harms may be valuable. Self-sampling for HPV testing can facilitate access to cervical cancer screening in low-resource settings, but more can be learnt about which characteristics of the self-sampling device or components of the test kit and supporting materials (eg, instructive images or video, inperson training or supervision) will increase acceptability among specific end-user groups like women living with HIV, from older age groups or with lower literacy. Work is needed to explore mechanisms and incentives for improved follow-up after screening, especially for populations self-sampling at home. The impact of large-scale use of HPV self-sampling for cervical cancer screening services on cost or resource use, and its cost-effectiveness, should likewise be examined. Operational research for scale-up of HPV self-sampling as part of self-care should be conducted, and clear guidelines for follow-ups for treatment should be developed.
The information presented in this review has been used to inform the development of WHO recommendations for self-care interventions for sexual and reproductive health and rights in relation to self-sampling for HPV testing. The benefits and harms of this intervention found in the present review can be considered along with values and preferences, resource use, human rights, and feasibility issues to inform the recommendation. It is hoped that additional research into the outcomes important to decision-makers will be conducted to fill the gaps identified in the current literature.
Conclusion
In summary, HPV self-sampling has the potential to increase uptake of cervical cancer screening. In meta-analysis, HPV self-sampling kits sent directly to women’s homes or offered by a health worker resulted in greater uptake of screening, compared with standard of care, although subsequent attendance of cervical cancer services for follow-up clinical assessment or treatment was generally low and similar to other modes of cervical cancer screening. In addition, the size and direction of effect vary significantly among studies, so more research is needed to evaluate the feasibility, effectiveness and cost-effectiveness of self-sampling in specific local contexts prior to large-scale implementation of self-sampling, especially in LMICs where coverage of effective screening algorithms is currently low.
Acknowledgments
We thank Laura Ferguson for her contribution to conceptualising this review, and Patricia Garcia, Gina Ogilvie and Nandi Siegfried for their thoughtful comments on the protocol. We thank Maribel Almonte, Nathalie Broutet and Anandi Yuvraj for reviewing an early draft of this manuscript. We also thank our Johns Hopkins Bloomberg School of Public Health graduate students (Melissa Camila Alamo, Chergai Gao Rittenberg, Priyanka Mysore, Holly Nishimura and Laura Graf) for their assistance in searching trial registries, screening citations and extracting data. Finally, we thank Janet Austin, Louise Cadman and Zahra Modibbo for graciously providing additional stratified data for our meta-analyses.
References
Footnotes
Handling editor Sanni Yaya
Contributors MN conceptualised the study. CEK and PTY designed the protocol, with feedback from HdV. PTY ran the search and oversaw screening, data extraction, and assessment of bias and quality of reporting. PTY and CEK conducted the meta-analysis. PTY drafted the manuscript. PTY, CEK, HdV and MN reviewed the draft, provided critical review, and read and approved the final manuscript. The corresponding author, as guarantor, accepts full responsibility for the finished article, has access to any data and controlled the decision to publish. The corresponding author attests that all listed authors meet the authorship criteria and that no others meeting the criteria have been omitted.
Funding We gratefully acknowledge financial support of the UNDP-UNFPA-Unicef-WHO-World Bank Special Programme of Research, Development and Research Training in Human Reproduction (HRP) and the Children's Investment Fund Foundation (CIFF). HRP was involved in the study design. The funders played no part in the decision to submit the article for publication, nor in the collection, analysis and interpretation of data. All authors had full access to all of the data (including statistical reports and tables) in the study and can take responsibility for the integrity of the data and the accuracy of the data analysis.
Disclaimer This article is part of a series proposed UNDP/UNFPA/Unicef/WHO/World Bank Special Programme for Human Reproduction (HRP) and commissioned by The BMJ. The BMJ retained full editorial control over external peer review, editing, and publication of these articles. Open access fees are funded by HRP.
Competing interests None declared.
Patient consent for publication Not required.
Provenance and peer review Not commissioned; externally peer reviewed.
Data availability statement Extracted data are available on request to the corresponding author